“We really do believe much harder times are coming from a reimbursement standpoint”, Daniel Morissette, Stanford Health Care CFO.
With value based model, the most unpredictable payment reform, in their list of financial challenges, CFOs point out their threats and decision making factors.
“We’re trying to evaluate all of the different services we have and evaluate how they will fit into what we believe is the future of healthcare”, Donald Longpre, CFO, North Ottawa Community Health System
“It’s not just the fact that we’re going to get paid less for what we’re doing. We’re also seeing a shift in business,” Chris Bergman, CFO, Christ Hospital Network, Cincinnati. CMS is nipping at little things”, Bergman said on what was worrying him.
When it comes to experience:
“You need to understand the issues, test your theories, and subtly verify your assumptions along the way,” says Tom Gibney, CFO of St. Luke’s Cornwall Hospital of Newburgh, New York, when asked about how experience plays a role in decision making. “The buck stops with you,” he says. “The board is looking to you for answers”, he quoted.
Reimbursement declines, physicians shortage, healthcare reforms and other factors have forced CFO’s to use their experience in answering how to recoup the losses and improve the organization’s cash flow.
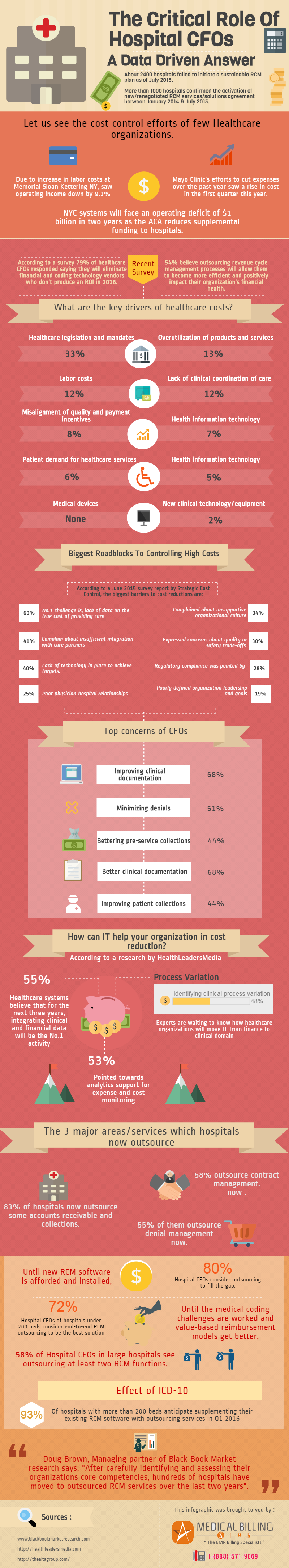
We organized the data collected from recent surveys to find out the challenges of healthcare CFOs in a value based era and the factors which influence their decision. Based on the results here’s a data driven answer.